PRICE protocol vs POLICE principle
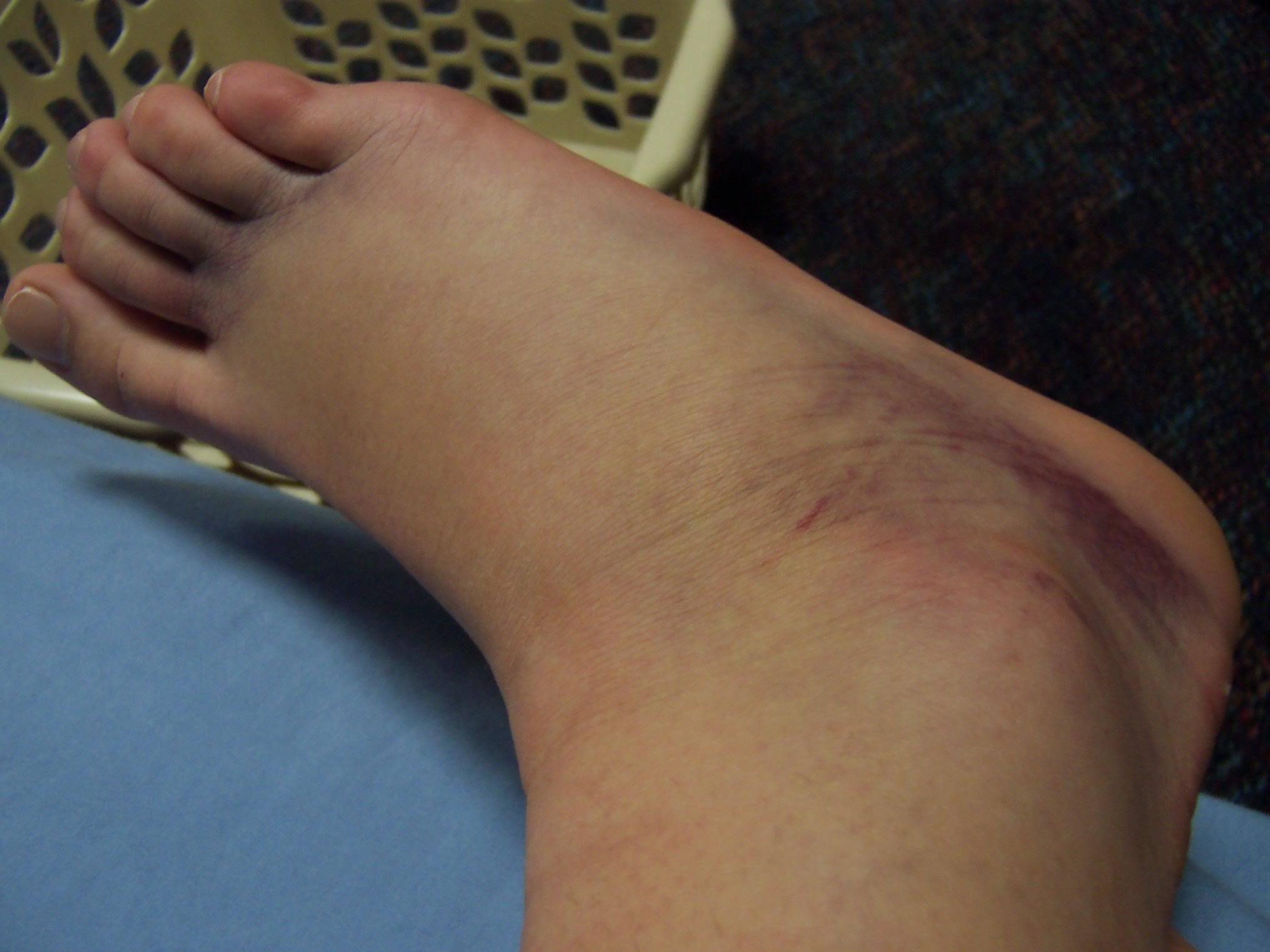
The acronym PRICE (Protection, Rest, Ice, Compression, Elevation) has been the standard of care in acute soft tissue management for decades. Recently, the literature that supports this theory has been reviewed, and many researchers and clinicians are recommending that the theory be modified to reflect current knowledge and practice. The new acronym suggested is POLICE (Protection, Optimal Loading, Ice, Compression, Elevation)
In order to understand the principles of soft tissue management, one must first have some basic understanding of the tissues involved and the body’s response to an acute soft tissue injury. Soft tissue injuries that are most commonly involved are listed below:
Tissues Involved
Bones and periosteum
Bones form the rigid framework of the body. The periosteum is the sensitive covering layer of the bone to which the tendons, capsules, and ligaments are attached.
Joints, Capsules, and Ligaments
Joints are the meeting places of two or more bones where movement takes place. A tough capsule encases all joints. Strap-like bands called ligaments reinforce capsules. Capsules and ligaments have little give and are common sites of injury.
Muscles and Tendons
Muscles are fleshy tissues, richly supplied with blood vessels. They contract and relax, both voluntarily and involuntarily. Tendons are strong, cable-like structures that connect the muscle to its bony attachments. The muscle-tendon unit is responsible for producing movement at the joints. Compared to muscles, tendons have much less blood supply and therefore often take longer to heal.
Bursa
Bursa are fluid-filled sacs strategically placed to reduce friction between layers of tissues, for example, between tendons and bones.
Nerves
Nerves are the electrical lines between the brain and the tissues of the body. They send messages to muscles, directing them to move parts of the body. They also provide the skin and all other tissues with sensations such as the sense of pain, sense of temperature, and sense of touch.
Blood Vessels
Blood vessels supply nutrition to the tissues of the body as well as remove waste products from the tissues of the body.When these vessels become damaged or inefficient, seeking care from Metro Vein Centers can provide specialized vein treatment to restore healthy circulation and prevent further complications.
Your Body’s Response to Injury
1. Soft Tissue Damage
Soft tissue damage occurs when excessive force or repetitive minor forces are applied to soft tissues excessively enough to cause soft tissue damage. This results in pain and may lead to a certain amount of internal bleeding and swelling.
2. Inflammation
The increase in the movement of plasma and white blood cells from the blood into the injured tissues causes inflammation, which is the body’s initial response to soft tissue damage.
The purpose of inflammation is to eliminate the initial cause of cell injury and clear out necrotic cells and tissues damaged by the original insult.
The signs of inflammation are:
• Pain
• Heat
• Redness
• Swelling
• Loss of movement
The inflammatory process may be present for as little as 3 and as much as 21 days, depending on the severity of tissue damage and the individual’s response to injury.
If the initial injury is not treated effectively, the inflammatory response could persist for an extended period of time. This often delays repair, leads to excessive scar tissue formation, causes loss of flexibility, strength, and function, and causes the tissues to become overly sensitive to normal stimuli (severe pain with the lightest touch or pressure on the injured tissues).
3. Repair
The repair phase begins within 2 days following injury, while the inflammatory process is still present. The repair process begins with the formation of new blood vessels around the edge of the injury site.
How does price help?
Protection and Rest
Protection and rest immediately following a recent injury are a no-brainer. When you feel pain following a recent injury, you should stop whatever you are doing. Take a few minutes to assess the damage and let the pain settle.
To prevent further damage, it is necessary to rest the injured part. To achieve this, you may need to immobilize the injured part with a brace and/or use a crutch to reduce weight on the injured area, if it is a leg, or a sling if it is an arm. When applying the principle of rest following an injury, it is not necessary to completely stop all activity for extended periods. In fact, even short periods of rest have been shown to be deleterious to the healing process, producing adverse changes in tissue morphology, biomechanical properties, and tensile strength. Usually, a few days of rest are adequate.
The injured part should only be rested to the extent that all painful activities are avoided. This is called relative rest. For example, if following a lateral ankle sprain walking does not cause any pain, continue to walk short distances as pain allows.
New research suggests early movement, or “optimal loading,” may accelerate the repair process (more on this later).
Ice and Cold Therapy
Both ice and cold therapy are very effective in reducing pain when the skin temperature is cooled to less than 15 oC for periods of 10–20 minutes. The effect of ice and cold therapies on the inflammatory process has recently been questioned. Studies on ice performed on animals have shown positive results in a reduction of cell metabolism and white blood cell activity. However, the studies of ice performed on humans have not been supportive.
The depth of the injured tissue, excessive layers of adipose, and the application of ice over bandages or dressings, according to researchers, prevent humans from reaching adequate cellular cooling to reduce cellular metabolism and white blood cell activity.
Ideally, ice or cold therapy should be applied immediately following an injury, as this helps to decrease pain and possibly inflammation. Ice therapy involves the use of ice to cool the injured area.
The following methods of applying ice are recommended:
- Place crushed ice with a little water in a plastic bag. Then place the bag containing the ice inside another bag and mold it over the injured area.
- Mold a packet of frozen vegetables over the injured area.
- Place a commercial therapeutic ice pack on the injured area, following the manufacturer’s instructions
Cold therapy provides less cooling to the injured area than ice therapy. It is therefore more suitable to apply cold therapy to children, the elderly, and persons with thin, fragile, or sensitive skin.
The following methods of applying cold therapy are recommended:
- Place a cold, damp flannel over the injured area. The flannel can be cooled by dipping it in ice water. When the flannel warms up, replace it with a cold one.
- Place the injured area in a bucket containing water and ice. This is useful if the injury is to the hand or foot.
- Place the injured area under cold, running water. This is useful for minor injuries or when other options are not available.
Guidelines for the application of ice and cold therapy
Ice can burn if the skin surface temperature reaches 0 °C. To avoid this, protect your skin with a layer of insulation before applying ice. Use a covering of oil or a damp cloth. Check your skin after a few minutes. If your skin has become white, stop the ice and try cold instead.
Both ice and cold may cause some initial discomfort. This should wear off in a few minutes. If, with the use of ice or cold therapy, your skin is becoming numb or increasingly painful, stop the ice or cold therapy and seek advice from a therapist.
Apply ice or cold for no longer than about 20 minutes. Prolonged application will be of no further benefit. To obtain the maximum benefit after a recent injury, apply ice or cold therapy every 3 hours.
Edema is one of the cardinal signs of acute inflammation after a soft tissue injury. Although some components of inflammation are essential for the healing process, prolonged edema is unwanted as it leads to increased tissue pressure, causing pain, movement restrictions, and muscle inhibition.
Edema happens when fluids build up in the interstitial space. Leaky capillaries, higher vasculature hydrostatic pressures, and a modified osmotic gradient after injury are the causes of this. If we can restore the pressure gradients at the capillary bed, we can prevent or limit the extent of edema.
Most practitioners try to achieve this using at least one of these approaches: compression and elevation. There is some suggestion that elevation and compression should not be used simultaneously. In fact, a few studies have reported that, when used together, they actually increase tissue girth after injury.
Compression
Compression is the application of pressure over the injured area by bandaging. This is an invaluable and often overlooked first-aid measure. It is the most effective way of reducing internal bleeding and swelling, particularly if applied within the first few minutes following an injury.
Guidelines for the application of compression:
- Use a bandage that will mold around the injured area, providing firm and even pressure. Elastic bandages are preferable to other types of bandages.
- Bandage a good distance below and above the injured area.
- Apply the bandage firmly and comfortably. If too tight, it may cause numbness; if too loose, it will be ineffective.
- A 15–30 mmHg compression garment may be substituted for elastic bandage wraps for some lower leg injuries.
- Remove the bandage before ice or cold therapy, and during elevation, reapply immediately afterwards. Rewrap in the mornings or whenever the bandage has loosened.
- For minor edema, the use of kinesiotext taping (or similar products) applied appropriately to the injured soft tissues may be of benefit and allow more mobility during use of the injured body part.
Elevation
Immediately following the injury, elevate the injured limb above the level of your heart to limit the development of swelling. Elevate your injured limb at every opportunity for as long as the swelling continues. Raising the injured limb above your heart level may be impractical at work and in other situations, but remember that some elevation is better than none at all.
For example, resting your injured ankle on a chair will still provide effective elevation. Gentle, pain-free muscle contractions while elevating your injured limb may enhance venous outflow and lymphatic drainage and should be performed when movement is tolerated (i.e., pumping of the ankle while elevating your leg).
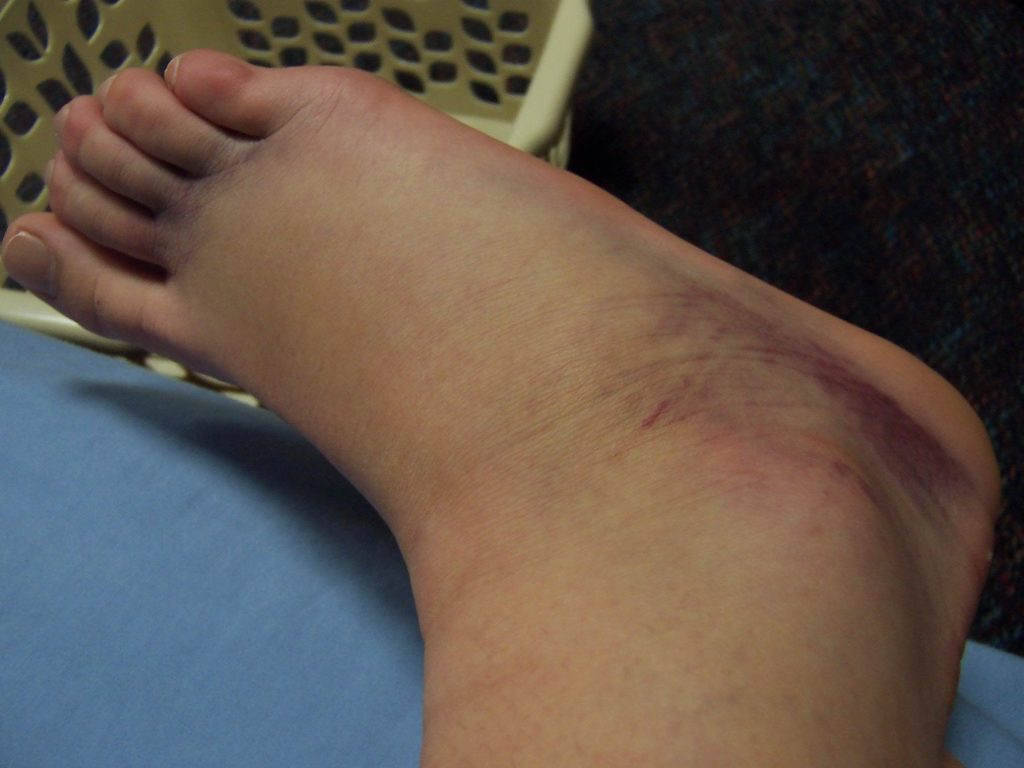
Implementing POLICE
The updated acronym POLICE aims to provide more nuanced and evidence-based recommendations for treating soft tissue injuries. Here is a breakdown of what each letter represents:
Protection: protecting the injured area from further harm. This may involve bracing, taping, crutches, etc.
Optimal loading: gradually and appropriately loading the injured tissue to encourage healing and prevent the detrimental effects of immobilization.
Ice: applying ice to help manage pain and swelling, especially in the acute inflammatory stage.
I. Compression: Using compression bandages or garments to limit swelling and hemorrhage.
Elevation: positioning the injured area above heart level to utilize gravity to drain excess fluid.
Education: Educating patients on their injury and care plan improves compliance. Providing a timeline and expectations helps patients stay motivated and progress appropriately during rehab.
Optimal Loading
As excessive rest following a soft tissue injury may be harmful and inhibit recovery, the secret is to find the” optimal loading” to enhance tissue repair without prolonging or intensifying the inflammatory process. Optimal loading means replacing rest with a balanced and incremental rehabilitation program where early activity encourages early recovery. Injuries vary, so there is no one-size-fits-all strategy or dosage. The optimal load is dependent on the predominant phase of healing (i.e., inflammatory or repair), the type of soft tissue involved (muscle, tendon, ligament, etc.), and the severity of the injury.
The behavior of pain with controlled movements and activities serves as a guide for the best loading strategy. In general, the controlled movements that are optimal to enhance recovery should slightly increase or produce familiar pain at the injury site but should gradually reduce in intensity with repetition or at least subside immediately upon rest from the controlled movement or activity.
As the injury progresses through the phases of healing, optimal loading of the injured tissues is achieved through more intense or rigorous activity. The aim of this strategy is to normalize newly formed scar tissue. The frequent adoption and progression of appropriate and controlled movements and activities in this manner have been shown to create a more elastic and stronger scar that is less likely to become re-injured with normal use of the injured body part.
Phases of Tissue Healing
There are typically three main phases of soft tissue healing:
- Inflammatory phase
- Proliferation phase
- Remodeling phase
Understanding which phase a tissue is in helps guide treatment and loading recommendations.
When to Seek Help
While many minor soft tissue injuries can be self-managed, some cases require medical attention. Seek help if:
- Severe pain/swelling
- Inability to bear weight
- Suspected fracture
- Persistent loss of motion or strength
- etc
Conclusion
Using evidence-based principles like POLICE can optimize healing outcomes. However, every injury response is unique, so care should be customized accordingly. Consulting a medical professional is wise in complicated or severe cases.
References
- American Heart Association. (2005). Circulation. Retrieved January 25, 2015.
- Bleakley, C. (2013, October). Acute soft tissue management update. SportEx Medicine (58), 16–19.
- Bleakley, C., Glasgow, P., & MacAuley, D. C. (2012). PRICE needs updating; should we call the police? British Journal of Sports Medicine, 46(4), 220–221.
- Lindsay, R., Watson, G., Hickmott, D., Broadfoot, A., & Bruynel, L. (1994). Treat your own strains, sprains, and bruises. Waikanae: Spinal Publications Ltd.





