What Can Physical Therapy Do For Carpal Tunnel Syndrome?
Compression of the median nerve at the wrist results in carpal tunnel syndrome (CTS), a common disorder.CTS is said to affect 1 out of every 20 Americans. CTS most commonly affects women older than 40 years and industrial workers who engage frequently in tasks that involve gripping. A number of risk factors for developing CTS have been identified. The following are a few:
- Previous wrist fracture or dislocation
- Inflammatory diseases (i.e. rheumatoid arthritis)
- Gender (more common in females)
- Diabetes
- Obesity
- Fluid retention (during pregnancy or menopause)
- Thyroid disease
- Kidney failure
- Work place factors (use of vibrating tools, frequent gripping , or wrist flexion)
The tunnel is a small opening about the diameter of your thumb. The transverse carpal ligament makes up the roof of the tunnel, and the small carpal bones of the hand make up the floor and sides. The median nerve, together with the flexor tendons of the fingers and the thumb, travel through this small opening.
Changing the cross-sectional size of the tunnel or making the contents inside the tunnel bigger can put pressure on the median nerve. This can cause numbness, tingling, and eventually weakness in the fingers that receive nerve supply from the median nerve. These fingers are usually the thumb and the second, third, and part of the fourth.

In the early stages of this disorder a person will be awakened at night with the symptoms of CTS and be forced to shake the hand out in order to gain relief. The person will often be symptom-free during the day. Later in the disorder, the person with CTS will frequently drop things due to weakness in the muscles supplied by the nerve, and the symptoms may become constant (present 100% of the day and night).
Diagnosis of CTS can often be made by history and simple clinical testing. A PT can obtain information regarding the exact location, severity, and quality of your hand symptoms. The PT will try to understand what daily activities seem to make your symptoms worse or better and ask questions about any relevant medical history, such as the presence of diabetes, rheumatoid arthritis, previous wrist trauma, and other potentially related symptoms such as neck and shoulder pain.
The cervical spine has long been thought to be involved in many CTS cases; therefore, the PT evaluation will consist of a screen of your cervical spine functions. If any abnormal findings are found, a full-blown cervical MDT evaluation may be administered to determine if it is causing your CTS symptoms or is a secondary disorder. The PT will evaluate your wrist and hand range of motion, grip strength, and sensation in your hand.
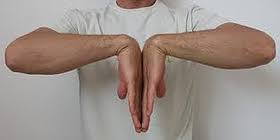
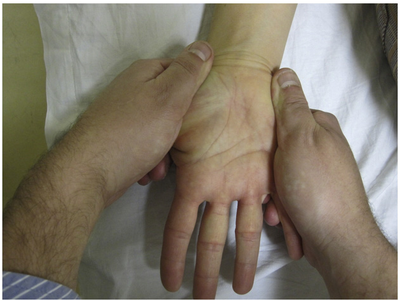
The PT will also perform a few special tests thought to confirm CTS as a diagnosis. These tests involve tapping your wrist over the tunnel and holding the wrist in an extreme flexed position for 60 seconds to see if your CTS symptoms appear. The PT may also refer to other health care providers to obtain radiography if trauma has occurred.
Referrals may also be made for electrophysiological studies. These studies are considered the gold standard to confirm the diagnosis of CTS. These studies include electromyography (EMG) and nerve conduction velocity testing (NCV).
Treatment of CTS Will Depend On The Stage Of The Disorder
If your CTS is in an inflammatory stage, which is characterized by constant pain that is easy to provoke and significantly disturbs sleep, treatment should include rest from aggravating activity, splinting, ice, and medications or injections to reduce inflammation.
When your CTS disorder gets to the dysfunctional stage, marked by symptoms that come and go depending on how much stress is put on the dysfunctional nerve and nearby tendons but go away quickly when you rest, you can usually get better with graded exposure to mechanical therapy. This will help restore the elasticity of the scarred tendon, tendon sheaths, and nerve.
Simple wrist extensions performed on a regular basis can help with mechanical therapy, which progresses to more complex upper extremity stretches intended to restore the median nerve’s mobility.
By doing resistance exercises and manual soft tissue mobilization techniques, you may also be able to strengthen the tendons that are affected and make the abnormal tendons and tendon sheaths smaller in size inside the tunnel.
The key to effective mechanical therapy for dysfunctional soft tissue is the frequent performance of a few procedures that adequately load the abnormal tissues to create a remodeling effect. These mechanical procedures will often need to be monitored and progress as the disorder recovers over several weeks or months.

Once your CTS has resolved, you should take steps to prevent recurrence of the disorder. The following may be beneficial:
- Take frequent breaks throughout the day and perform the same stretches for your wrist that helped resolve your CTS
- Take frequent breaks and stretch your neck, shoulders, and back
- When working with your hands keep you wrist in a neutral position. Avoid working with the wrist bent downward or upward.
- Modify your writing instruments and tools with oversized grips
- Reduce your force when gripping instruments/tools when possible
- Avoid or minimize use of vibrating tools.
- Improve your posture when sitting, standing, and working. Pay attention to your low back, neck and shoulder position. Maintain these body parts in a neutral position to avoid any abnormal stresses. If this cannot be avoided. Frequently alter your work posture and activities (sit to stand, stationary activity to dynamic activity).
- Maintain good general health. Staying physically fit and maintaining a healthy weight may help control diseases and conditions that may contribute to the onset of CTS (obesity, diabetes, arthritis, etc.).





