How many knee replacements per year?
Joint replacement surgery is one of the most successful interventions in all of medicine. The American Joint Replacement Registry’s (AJRR) 2022 annual report compiled data on over 2.8 million hip and knee replacement procedures performed in the United States. Here is a deep dive into the statistics and facts surrounding these life-changing operations.
By the Numbers
- 790,000 – The approximate number of knee replacements performed in the U.S. each year
- 450,000 – The approximate number hip replacements performed annually
- 90% – The percentage of joint replacement recipients reporting excellent pain relief and restored quality of life
- 20+ years – The typical longevity of modern joint implant components
- 1.3 days – The average hospital length of stay following knee replacement
- 1.4 days – The average stay after a hip replacement
- 65.7 years – The average age of a patient undergoing hip replacement
- 67.2 years – The average age for knee replacement patients
- 58.5% – The percentage of joint replacements performed on female patients
- 36 – The average number of knee replacements performed per high-volume surgeon in 2021
- 27 – The average number of hip replacements per high-volume surgeon
These statistics confirm joint replacement as one of the highest-volume, most successful elective surgeries aimed at dramatically improving patients’ comfort and quality of life.
Who is a good candidate for joint replacement?
Joint replacement surgery is typically only recommended after other medical treatments for arthritis have failed to provide adequate relief. Good candidates are individuals with:
- Advanced, end-stage arthritis in the hip or knee
- Significant, persistent joint pain that impacts quality of life
- Loss of joint function and mobility
- Failure to achieve pain relief or functional improvements with medications, injections, physical therapy, or assistive devices
The decision about joint replacement relies heavily on the patient’s reports of pain, mobility limitations, and reduced quality of life due to their arthritis. Candidates should be healthy enough to tolerate anesthesia and participate in postsurgical rehabilitation. Patients’ physicians will assess their medical fitness for surgery.
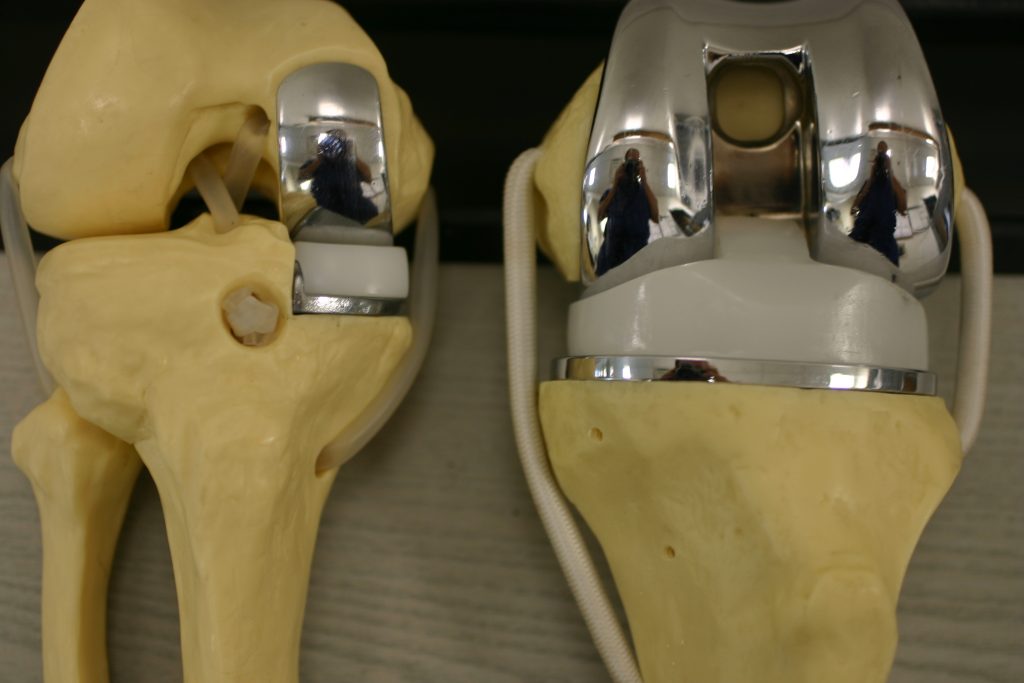
What does the surgery entail?
During joint replacement surgery, the orthopedic surgeon removes the arthritic joint surfaces and damaged bone. These parts get replaced with artificial joint components made of metal alloys, plastics, and sometimes ceramics.
The most common joint replacements are:
Total knee replacement: Damaged surfaces get removed from the thigh bone, shin bone, and kneecap. These bones get resurfaced with metal and plastic components shaped like the original knee parts. Depending on the implant style, the surgeon may also replace or spare the posterior cruciate ligament in the center of the joint.
Total hip replacement: The hip socket and femoral head get replaced with new synthetic parts. The hip socket component commonly has a metal outer shell with a plastic liner. The femoral component has a metal stem that fits inside the femoral bone and a metal or ceramic ball on top that articulates against the socket.
The surgery usually takes 1-2 hours. Patients typically stay 1-3 days in the hospital afterward for pain management before going home to recover.
Preventing the Need for Surgery
While joint replacement reliably relieves pain and restores function, undergoing any surgery has inherent risks. Patients can delay or avoid joint replacement surgery through comprehensive conservative arthritis treatment including:
- Medications like NSAIDs, steroids injections, disease-modifying antirheumatic drugs (DMARDs)
- Low-impact exercise like walking, swimming, stationary biking
- Weight loss if overweight
- Braces, ambulatory aids, shoe orthotics
- Physical or occupational therapy
Such treatments can help patients maximize their joint health and quality of life before resorting to surgery. However, joint damage in end-stage arthritis is irreversible without replacement. Conservative measures often eventually fail to provide satisfactory relief at which point patients and their doctors can discuss surgery.
Recovery and Life after Surgery
The road to recovery starts immediately after surgery. In the hospital, patients begin gentle movement exercises and walking as soon as possible. At home, they continue physical therapy to restore range of motion, strength, and the ability to perform daily activities. Assistance from a physical therapist or athletic trainer is extremely valuable in ensuring optimal recovery.
With dedicated rehabilitation, joint replacements provide excellent pain relief and huge quality-of-life improvements for more than 90% of patients. Most recipients regain the ability to participate in low-impact activities like walking, swimming, golfing, doubles tennis, and light hiking. Higher-impact sports like singles tennis, basketball, and jogging are discouraged as they place excessive wear and tear on implants.
Modern joint replacement components last upwards of 20 years for most patients before wearing out. Some people outlive their implants and require revision surgery to install new ones later in life. Such revise operations tend to have more variable outcomes than initial joint replacements.
Conclusion
For hundreds of thousands suffering from severe hip and knee arthritis each year, joint replacement surgery is a safe and effective way to get back cherished parts of life diminished by pain and immobility.
Candidates should meet with their primary care doctor and orthopedic surgeon to discuss their symptoms, exam and imaging findings, treatment options, and preparation to optimize their surgical and postsurgical health. With patience through recovery, most joint replacement recipients can anticipate greatly improved comfort and the ability to participate in daily and recreational activities.





